APPROACH TO DENTAL AGED PATIENT WITH ALZHEIMER’S DISEASE
SUMMARY:
Alzheimer’s disease (AD) is a dementia that is Characterized by neurodegenerative, progressive and irreversible, is a condition That Occurs in elderly Patients and is the most common cause of dementia in this population. The etiologic factors “are multiple and the evolution is slow but progressive. The this segment of the ever-growing population, the literature review next wants to familiarize with the Dentistry the clinical features of the illness and the way of focusing the treatment plan in this kind of Patients Described in Patients with AD, there is poor oral hygiene and the higher prevalence of oral diseases, due to the inability to perform Adequate oral hygiene. There are five important elements in the oral health care: SYMPTOMS, oral examination, treatment, the role of caregiver versus oral health and the role of the dentist.
Keywords: Alzheimer’s Disease, Oral Hygiene, Dental Health, Oral Care in Older Adults.
INTRODUCTION:
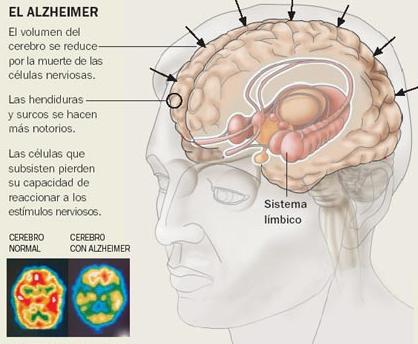
Alzheimer’s disease (AD) is a dementia that is characterized by gradual onset, insidious and irreversible neurodegenerative disorder, was first mentioned in 1906 by German pathologist Alois Alzheimer, who described the disease as a progressive disorder of the central nervous system causing characteristic lesions in the brain and diffuse loss of neurons in the hippocampus and neocortex. (Kocaelli H, Yaltitrik M, Yargic I Özbas H., 2002)
There are currently worldwide between 17 and 25 million people with Alzheimer’s disease, which corresponds to 70% of all diseases that affect the geriatric population. Thus, Alzheimer’s disease is the third leading cause of death in developed countries, exceeded only by cardiovascular disease and cancer. (AF Miranda, 2008)
In dentistry, for example, it is rare that professionals have adequate training to the needs of these people ateneder therefore this paper reviews the relevant aspects related to the oral health of patients with Alzheimer’s. (AF Miranda, 2008)
The etiology of dementia is complex and may be associated with factors such as age, family history, vascular problems disease, immune deficiency, metabolic disorders, genetic factors, brain trauma, tumors, infections, and factors that compromise the nutritional quality of life (drugs, hypertension, smoking and alcohol consumption). (Goiato MC, 2006).
10 Warning Signs of Alzheimer’s disease:
(Http://alzheimeruniversal.blogspot.com/2010/09/10-signos-de-alerta-del-alzheimer.html)
1. – Memory loss: The disappearance of short-term memory (forgetting things recently learned) is an early sign of dementia.
2. – Difficulties in implementing family labors: By completing routine activities of daily life begins to be difficult for the subject, we must be alert and check whether it is a pattern that is repeated day after day, and how.
3. – Problems with linguagen: people with Alzheimer’s often exchange words with no rhyme or reason, both in speech and writing, making his speech difficult to understand.
4. – Temporal and spatial disorientation: Alzheimer’s patients may be lost even in his own backyard and forget how they got there, not knowing how to get back too.
5. – The loss or decline of common sense: Wear long-sleeved blouses on a hot day or a short on a cold day, it can reveal the loss.
6. – Problems with abstract thinking: Challenges to run the complex mental processes, like forgetting what numbers are or what they do.
7. – Problems of location of objects: a person places the objects in places that do not (for example, a shoe in the fridge).
8. – Changes in mood and behavior: Changes in mood as the being of the individual, or how to behave. You can stay completely calm in a moment of rage and exploded seconds later.
9. – Changes in personality: unexpected changes in lifestyle of the individual can also be a sign of Alzheimer’s disease. For example, if a person becomes suspicious, confused, often suspicious of others, etc..
10. – Loss of initiative and activity: A person becomes a liability, who spends hours watching television, sleeping too much or do not want to do routine tasks.
10 signs that do not involve Alzheimer
1. – Forgetting names is perfectly associated with advanced age and is not a sign of Alzheimer’s disease.
2. – To forget why we went into a room and we would say, is something that can happen to anyone, especially if this is the elderly.
3. – Having trouble finding the right word at some point in the speech.
4. – Forget the days of the week or day of the month that we’re right.
5. – Implement an occasional questionable action or activity.
6. – Let us temporarily to another place or forget a wallet or keys.
7. – Finding it hard to read a book of accounts or any text or document involving a judicious exercise of concentration and analysis.
8. – If you feel sad or moody.
9. – One must keep in mind that people change their personality in some respects, with age.
10. – Feeling sick of work duties and / or social.
Alzheimer’s Disease
Alzheimer’s disease has a clinical course that ranges from 8 to 10 years from discovery in the initial phase. The individual characteristics of each stage of the disease are crucial for developing a treatment plan appropriate oral health needs of the patient.
The investigation should be thorough, through full and detailed medical history and contact your doctor dopaciente should be established from the outset. The dentist must use the consent form signed by the patient, if not dependent. Those responsible if the patients can not take their actions more often when it has suffered injunction. Thus, like other health areas involved in this context, the dentist should direct their actions according to the specifics of each patient, depending on the peculiarities of each phase of the disease: early, middle and end.
Initial phase
The early stages of the disease that can last 0-4 years and are characterized by memory loss, such as forgetfulness, lack of ability to learn and retain new information, communication problems (language), judgmental errors and progressive difficulty in performing normal daily activities such as cleaning actions. At this stage of the disease, patients usually present a clinical picture which hinders accurate diagnosis. The patient, despite continuous forgetfulness characteristic of the disease, may be undergoing treatment at the clinic. All the preventive management should be done at this stage, because with the progression of the disease, begins the difficult trip to the office. This phase is the right time to do any kind of dental procedures and prepare the best possible conditions of the stomatognathic system, compared to the evolution of the disease. It is the responsibility and competence of dentist tailor the oral environment, to improve the physiology of the stomatognathic system and, especially, to guide the patients themselves, carers and relatives concerning the maintenance of oral hygiene through proper cleaning techniques. The electric toothbrush is an important technical support, however, its use depends on the ability of the family caregiver and guardian. Among the practices of oral health care is the guidance on oral hygiene, plaque control, the functional character restorations, occlusal adjustment, the rebasing of dentures and periodontal treatment. The treatment planning and the preservation of clinical conditions must anticipate the future oral health problems in these patients. Importantly, the training of caregivers and family members are more accepted in this phase, so the investment in treatment and maintenance of oral health is of utmost importance. Over time, increases the difficulty of cleaning and patient acceptance to perform clinical procedures.
Intermediate phase
With disease progression, the intermediate phase lasts 2 to 8 years after diagnosis. Cognitive losses occur frequently additional disturbance in language, repetition of words, interference with occupational activities, inability to self-care, high risk of secondary accidents, unrest, lack of understanding and aggressive attitudes. The dentist should be very aware that at this stage since there are difficulties in language expression, especially in relation to pain. The patient needs constant companion on trips to the dentist. It starts, then a phase of semi-dependence on activities of daily living, which creates need for help in implementation of oral hygiene, an essential condition for maintaining conditions favorable to good health. It also initiates the establishment of the lack of cooperation from the patient to accept dental interventions. From this stage you can start the dental domiciled. In this context, there is greater interaction with the patient, family and all health professionals. The dental plan is characterized by attention to key requirements, in order to remove possible sources of infection such as periodontal problems, and especially the elimination of any possible determining factor of pain. Are common traumatic ulcers caused by poorly fitted dentures and fractured teeth. There is also possibility of performing dental procedures under sedation. In this case, planning should be done in conjunction with the physician. The conscious sedation with nitrous oxide, carried out by duly qualified dentists is a viable alternative that can be performed in office setting. Another alternative is the prescription of benzodiazepines as anxiolytics, with the consent of a doctor, preferably. These actions considerably easier to dental intervention and avoid the stress of patient11, 16. Poorly fitted dentures, poorly sanitized are of questionable use in this phase. The removal of implants should provide the favorable condition of oral health and prevent the occurrence of possible accidents, such as aspiration or swallowing them. Caregivers should be trained to the daily responsibility of oral hygiene and researchers symptomatic of the key information as objectively as possible about the patient appears to need the dentist to have knowledge and ability to function at home, caregivers and family members present when unprepared for the dental management of these patients.
Final phase
The final or terminal phase of illness, lasting 60 to 10 years, is determined by the profound disorientation, apathy, dependence, total urinary and fecal incontinence, complete loss of recent memory. It can also occur aggressiveness and anxiety. At this stage it is common to the risk of malnutrition. The gradual progress of the patient leads to coma and death. The dentist is part of a cycle of attention to the health of the patient, is of great importance to its work, like other areas of health. A great discussion with the professionals about the actual need of dental care has decisive character in the evolution of the disease. The minimum requirements for oral health should be prioritized. We know the relationship of dental foci of infection and its effect on general health as well as deaths related to aspiration pneumonia, often due to lack of oral conditions favorable for these patients. The elderly dependents at home, nursing homes, hospitals and in intensive care, deserve specific attention and permanent. The dentist must be inserted in preparing the plan of treatment and maintenance of oral health status of these patients.
Complex and lengthy treatments should be avoided in this phase. The dentist must act solely in the removal of foci of infection and pain symptoms that affect the general health condition of the patient. The intention at this stage is to provide quality of life for the patient. Some procedures under supervision, proper technique and adaptation of dentists to this new context, which determine the number of oral health practices designed in a way directed to the needs of the moment. The use of expanders mouth, mouth openers, overhead lighting and appropriate instruments are useful in performing clinical procedures. It appears that most caregivers do not present adequate training to perform certain procedures concerning the maintenance of oral health of these patients.
The dentist must be present regularly in the clinical actions and decisions to improve the quality of life of patients, always maintaining the integrity and providing comfort and well-being of the same.
Alzheimer’s Dentistry
Beyond the health care team is essential and necessary for maintaining oral health of the elderly. Faced with this aging population comes the need to insert the dentist in multidisciplinary teams. Thus, it is interesting that the professional who wishes to meet older people go through specific training in order to relate in an inter and multidisciplinary, whether in private practice, home, as hospital (operating room, ICU, ward). Moreover, the dentists, as an educator in health promotion, has importantena role and relationship with family caregivers of Alzheimer patients, as it can and should encourage them and train them to maintain oral health, thus providing the quality of life.
Dental Management
Thanks to the progressive increase in life expectancy in modern societies, the dentist is and will be more frequently in the future, with significant population growth warrants geriatric dental care. Therefore the formation of dental clinics to address the conditions of this population is essential to provide a quality service, and one of the most common conditions in this growing population of Alzheimer’s disease. (Miranda AF, Montenegro FLB, Lia IN MPAF Miranda, 2008)
The treatment plan for a patient with AD should be designed according to the severity of the disease and always in concert with family members or people who are responsible for patient care. Importantly, as the disease progresses the patient’s oral condition progressively worsened, especially with regard to oral hygiene (Bridgman AM, Wilson MA. 2000) Therefore, if we see a patient in the early stages of disease needs to expect this deterioration to urgent prevention measures (topical applications of fluoride, chlorhexidine rinses, etc.). and frequent appointments for scaling and / or prophylaxis.
It is essential to visit the dentist regularly at these centers to prevent the presence of oral foci of infection which may aggravate the patient’s systemic condition. Relatives usually feel much more relaxed and confident when your dentist fully understands the details of the disease and can give specialist help to patients with Alzheimer’s. (Kocaelli H, Yaltitrik M, Yargic I, 2002).
FINAL CONSIDERATIONS:
The dentist should be aware of the different stages of Alzheimer’s disease and their characteristics to draw attention to the oral health of their patients individually. And possess the skills to perform the treatment at different stages of the disease. Dentist Participation in the EA is essential, in addition to the health team is also necessary to maintain oral health of seniors.
With the increase of the aging of the population, it is important that the dentist you want to meet older adults have a specific multidisciplinary training, either in private practice, as in the hospital. Moreover, the dentist, as an educator in health promotion plays an important role in the relationship with caregivers and relatives of Alzheimer patients, as it must encourage and train to maintain oral health, providing quality of life.
The dentist should be able to tailor treatment to the elderly population dependent on a multidisciplinary approach, respecting the individuality of the patient, always evaluating medical procedures and the family context.
Dental actions should focus on eliminating risk factors (inflammation, infection and pain) of the shares of minimal intervention and is considered safe.
It should be noted that shortly after the diagnosis of dementia, the patient should be referred to the dentist for an evaluation, because with the passage of time and the evolution of the disease, dental procedures are more difficult to perform, leading to possible confusion of the medical institution and unnecessary drugs.
The Odontogeriatra has much to say in a multidisciplinary team of health assessment, planning and execution of services focused on the elderly with dementia.
It is important to maintain the dental history in regard to medical history and medications to avoid complications such as postural hypotension product of antihypertensive drugs, adverse interactions with epinephrine or over-sedation. The salivary dysfunction is also a side effect of certain drugs used in the treatment of geriatric patients. Certain antihypertensive drugs, for example, can cause xerostomia, whereas in contrast, cholinesterase inhibitors may cause salivation
Intravenous sedation or general anesthesia may be necessary in certain procedures or stages of the disease, this increases the cost of treatment and may become a problem in our country where a high percentage of Alzheimer’s patients are low income or are abandoned by their relatives in institutions that do not have the minimum conditions to house them, while others remain in poverty.
References:
Bidzan L, Biliekiewicz A, Turczynski J. Preliminary assessment of ginkgo bilobae (Ginkofar) in patients with dementia. Psychiatr Pol. (2005); 39(3): 559-66.
CORRÊA, A. C. O. Envelhecimento, depressão e Doença de Alzheimer. Health, 1, p. 227, 1996.
EVANS, D.A. Prevalence of Alzheimer disease in a community of older adults, J. Am. Med. Assoc. v.262, n.6, p.2551,
Graziano KV, Maia FM. Principais acidentes de causa externa no idoso. Gerontologia. 1999;7(3):133-9.
Ghezzi E, Ship JA, Arbor A. Dementia and Oral Health. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. (2000); 89: 2-5.
Goiato MC, Santos DM, Barão VAR, Pesqueira AA, Gennari Filho H. Odontogeriatria e a Doença de Alzheimer. Pesq Bras Odontoped Clin Integr 2006;6(2):207-212.
Klinger T, Ibach B, Schoenknecht P, Kamleiter M, Silver G, Schroeder J, Mielke R. Effect of donepezil in patients with Alzheimer’s disease previously untreated or treated with memantine or nootropic agents in Germany: an observational study. Curr Med Res Opin. (2005);21(5):723-32.
Kocaelli H, Yaltitrik M, Yargic I, Özbas H. Alzheimer’s Disease and dental management. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. (2002); 93: 521-4.
Little JW. Dental management of patients with Alzheimer’s disease. Gen Dent. 2005;53(4):289-96.
Leal MCC, Marques APO, Marino JG, Austregésilo SC. Perfil de instituições asilares no município do Recife, PE, Brasil. Ver Bras Geriatr Gerontol. 2006;9(3):39-48. interesse clinico. São Paulo: Artes Médicas; 2002. p.110-1.
Miranda AF, Montenegro FLB, Lia EN, Miranda MPAF. Demência senil(Alzheimer): intervenção odontológica multidisciplinar em nível de consultório e domiciliar – Relato de caso clínico. Rev Eap/Apcd Sjc 2008; 10(1):11-13.
Nitrini R, Caramelli P, Bottino CMC, Damasceno BP, Brucki SMD, Anghinah R. Diagnóstico de doença de Alzheimer no Brasil. Arq Neuropsiquiatr. 2005;63(3-A):720-7.
Reiman EM, Caelli RJ. Alzheimer’s Disease. Maturitas. (1999); 15:31: 185-200.
Saxe SR, Wekstein MW, Kryscio RJ, et al. Alzheimer’s Disease, dental amalgam and mercury. JADA. (1999); 130: 191-9.
Scheneider LS. Treatment of Alzheimer disease with cholinesterase inhibitors. Clin Geriatr Med. (2001); 17: 337-58.
SMITH, M. A. C. Doença de Alzheimer. Revista Brasileira de Psiquiatria; 21, s2, p. 3-7, 1999.
Southern Association of Institutional Dentists. Clinical concerns in dental care for persons with mental illness: self-study. SAID. 2007;9:1-16
Van Reekum R, Simard M, Fracnik K. Diagnosis of dementia and treatment of Alzheimer’s disease. Pharmacologic management of disease progression and cognitive impairment. Can Fam Physician. (1999); 45: 945-52.
Varjão FM. Assistência odontológica para o paciente portador da doença de Alzheimer. Rev Odonto Ciência 2006;21(53): 284-288.
Zuluaga M, Javier D. Manejo odontológico de pacientes com demencias. Rev Fed Dent Colomb 2002;203:28-39.
(http://alzheimeruniversal.blogspot.com/2010/09/10-signos-de-alerta-del-alzheimer.html)
http://alzheimeruniversal.blogspot.com/2010/09/10-signos-que-no-implican-alzheimer.html)




 English
English  Spanish
Spanish  Portuguese (Brazil)
Portuguese (Brazil)